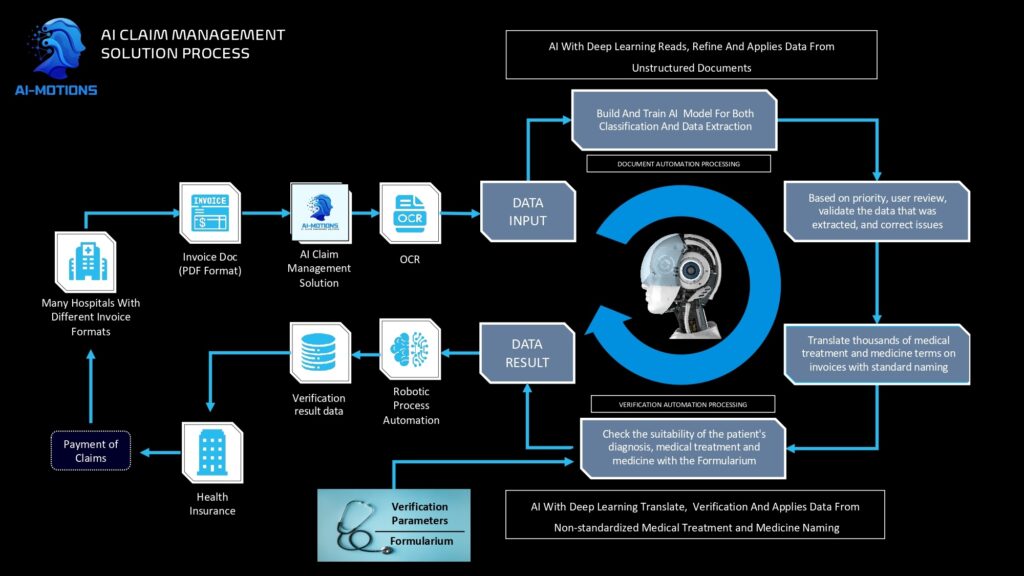
Modules
01
Claim Intake Module
AI-driven form processing, text input, and document scanning (OCR).
02
Claim Validation Module
Verifies policyholder details, coverage, and claim eligibility using rule engines and AI.
03
Fraud Detection Module
Uses machine learning to flag suspicious or inconsistent claims for review.
04
Automated Decision Engine
Applies business rules and AI models to approve or escalate claims.
07
Analytics & Reporting Module
Provides insights, trends, and performance metrics using AI-powered dashboards.
05
Document Management Module
AI categorizes and extracts relevant data from claim-related documents.
08
Customer Self-Service Portalule
Allows users to file, track, and update claims through an intuitive interface, often supported by virtual assistants.
06
Notification Module
Sends real-time updates to customers via chatbots, email, or SMS.
09
Integration Module
Connects with external systems like CRMs, payment gateways, and policy database.